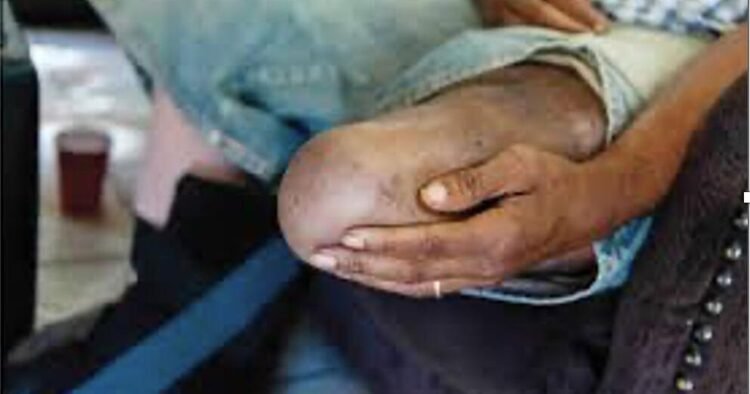
Just recently, I had two patients in my office, and I was very concerned about their feet and the possibility of them having to have an amputation. Both patients were diabetics and had problems with their feet. One had a wound for some time that was not healing, and the other had a minor injury to their foot. Both also had poor blood flow to the feet.
Every year in April, we shed light on amputation prevention and increase limb loss awareness, focusing on the latest care and collaboration needed to prevent them. The Amputee Coalition highlights the importance of early detection of vascular disease and patient education. Poorly controlled diabetes can lead to amputations, usually of the toes, feet, or legs. Research from the International Diabetes Federation showed that people living with diabetes feared amputation more than death.
Globally, about one million limbs are amputated every year. In The Bahamas, we are not sure, but it is estimated that 1,000 people lose a limb to amputations every year. These amputations also increase lifetime hospital care cost by $150,000 each. As high as 80 percent of non-traumatic lower limb amputations happen due to diabetes complications. An individual who has had an amputation has a worse chance of five-year survival than someone with coronary artery disease, breast cancer, and colorectal cancer. Eighty-five percent of all amputations are preceded by an ulcer and can potentially be prevented. Fifty-four percent of people living with limb loss have vascular disease, the most common cause.
Eighty-five percent of diabetes-related amputations are preceded by an ulcer and, therefore, can be prevented – if we prevent the ulcer or heal it quickly. Here are some simple steps that people living with diabetes and their health care providers can take to help prevent amputations.
Diabetes complications can include nerve damage and poor blood flow. Nerve damage can keep people with diabetes from feeling injury to the feet, or skin sores, or ulcers. Less blood flow can make it harder for these sores to heal, leading to infections and amputations.
Good diabetes control and regular foot care help prevent ulcers and serious foot sores that are hard to treat and may result in amputation. The good news is that managing your diabetes and taking care of your feet can help prevent foot ulcers and amputation.
Foot ulcers need care right away. An ulcer that won’t heal harms tissue and bone. It may lead to surgical removal, called amputation – of a toe, a foot, or part of a leg.
The following raise the risk of amputation in people with diabetes – high blood sugar levels, smoking, nerve damage in the feet, called peripheral neuropathy, calluses or corns, changes in the shape of the feet, poor blood flow to the arms and legs, called peripheral artery disease, history of foot ulcers, past amputation, kidney disease and high blood pressure.
Preventing foot ulcers: Managing your diabetes is the best way to prevent complications, including foot ulcers. This includes having good eating and exercise habits, checking your blood sugar often, and taking your medicine as prescribed.
Good foot care includes the following:
Looking at your feet daily: Check your feet once a day for blisters, cuts, cracks, sores, redness, tenderness or swelling. If you have trouble reaching your feet, use a hand mirror to see the bottoms of your feet. Put the mirror on the floor if you can’t hold it or ask someone to help you. People at high risk of foot ulcers also may use a thermometer to measure the temperature of the skin. A temperature higher than four degrees might mean the start of a foot ulcer at that location.Wash your feet daily: Wash your feet in warm water once a day. Don’t use hot water. Dry your feet carefully being sure to dry between the toes. Use a pumice stone to gently rub the skin where calluses form. Use a moisturizing cream or lotion on the tops and bottoms of your feet to keep the skin soft. Preventing cracks in dry skin helps keep germs out.
Don’t remove calluses or other foot growths yourself: To keep from hurting your skin, don’t use a metal nail file, nail clipper or scissors on corns, calluses, or warts. Don’t use chemical wart removers. See your healthcare professional or podiatrist to treat these issues.
Cut your toenails with care: Cut your nails straight across. Gently file sharp ends with an emery board. Ask someone for help if you can’’ trim your nails yourself.
Don’t go barefoot: To keep from hurting your feet, don’t go barefoot, not inside or outside.
Wear clean, dry socks: Wear socks made of fabric that pulls sweat and moisture away from your skin. This includes cotton and special acrylic fibers, but not nylon. Don’t wear tight socks, they lower blood flow to the feet. Don’t wear socks with seams that could rub and cut your skin.
Buy shoes that fit well: Buy comfortable shoes that support and cushion the heel, arch and ball of the foot. Don’t wear tight shoes, high heels, or narrow shoes that crowd your toes. If one foot is bigger than the other, buy shoes in the larger size. Remember to buy shoes in the afternoon to ensure a perfect fit. Wear the right shoes for the right activity. According to your foot condition, diabetic shoes may be recommended. These shoes fit the shape of your feet, cushion your feet, and make sure weight is the balanced on both feet.
Don’t smoke: Smoking makes it harder for your blood to flow through your body especially down to the feet. It also lowers the amount of oxygen in your blood. Smoking can make wounds worse and slow healing. Talk to your healthcare professional for help with quitting smoking, for your health.
Schedule regular foot checkups: Your podiatrist will examine your feet for signs of nerve damage, poor blood flow or other foot issues. Your should have your feet examined at least once per year and more often if your feet are at high risk of foot ulcers and amputations.
Contact your podiatrist or healthcare professional as soon as possible if your feet have ingrown toenails, blisters, plantar warts, athlete’s foot, open wound or bleeding, swelling, pain, warmth or change in skin color, a bad odor or smell, a wound that is slow to heal or lasts longer than one to two weeks, a sore that’s getting bigger and deeper.
If you suspect you have peripheral artery disease (PAD), diabetes with non-healing wounds, you are at high risk for an amputation, see a podiatrist or vascular doctor as soon as possible. You will need further testing, evaluations and treatment to prevent an amputation.
- For more information email info@familyfootcentre.com or visit www.foothealthfacts.org or www.footlogix.com. To see a podiatrist visit Family Foot Centre on #45 Daffodil Avenue, Independence Highway or call 605-3668; Bahamas Surgical Associates Centre at Hill Top Medical, telephone 603-1814/5. In Grand Bahama visit Lucayan Medical Center on East Sunrise Highway or call 373-7400.